Ultherapy is widely regarded as one of the most powerful non-invasive treatments for lifting and tightening of the face and neck without downtime. Ultherapy uses microfocused ultrasound to generate a thermal effect under the skin. Ultherapy penetrates deeply and precisely into the foundational layers of skin tissue, bringing about tightening and lifting of the brows, cheeks, jawline, and neck.
Ultherapy
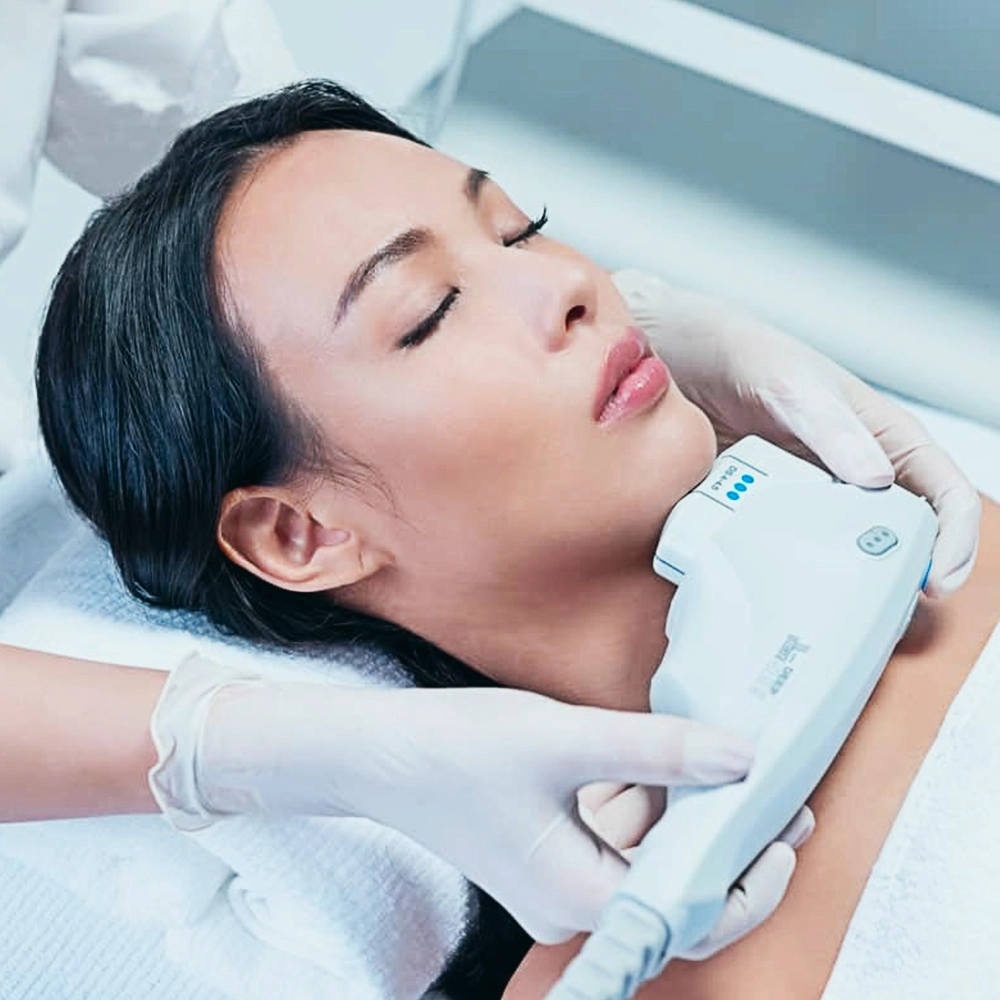
Collagen is an important natural structural protein that confers support and volume to the skin. As we age, our collagen and elastic tissue gradually degrade in strength and quality. Ultherapy jumpstarts a repair and renewal process that strengthens collagen and elastic tissue.
Ultherapy is the only nonsurgical cosmetic procedure that uses ultrasound to specifically target the foundational layer of facial tissue that doctors address in surgery. The use of ultrasound also enables us to actually see the layers of skin we are treating, allowing the energy to be delivered precisely to where it will be most productive.
Ultrasound energy has a proven track record, with its use in medical imaging for over 50 years. In addition, the procedure has been cleared by the FDA after demonstrating safety in clinical studies, and tens of thousands of treatments have been performed worldwide without any significant adverse events.

Ultherapy is ideal for people who are starting to notice some laxity and sagging of their face, jawline and neck. Ultherapy is also very helpful for reduction of lines and wrinkles on the upper chest/décolletage.

A full face and neck treatment usually takes about 60 minutes.

Comfort thresholds vary from patient to patient, but there can be some discomfort while the energy is being delivered, which is temporary and a signal that the collagen-building process has been initiated. We will take measures to make the experience as comfortable as possible, and this may involve the use of numbing creams and painkillers.

After Ultherapy, one will enjoy natural looking and noticeable results which are best seen around 2 to 3 months after the treatment. Results usually last for 1 year of more. One can consider having another Ultherapy treatment about 2 years later to keep pace with the ageing process.

There may be slight redness for a few hours following the treatment, and it’s not uncommon to have slight swelling, tingling or tenderness for a few weeks, but these are typically mild and temporary. There can be other post-procedural effects such as bruising and small areas of numbness but these are less common and temporary.
Hair Loss
Common hair loss problems are discussed below.
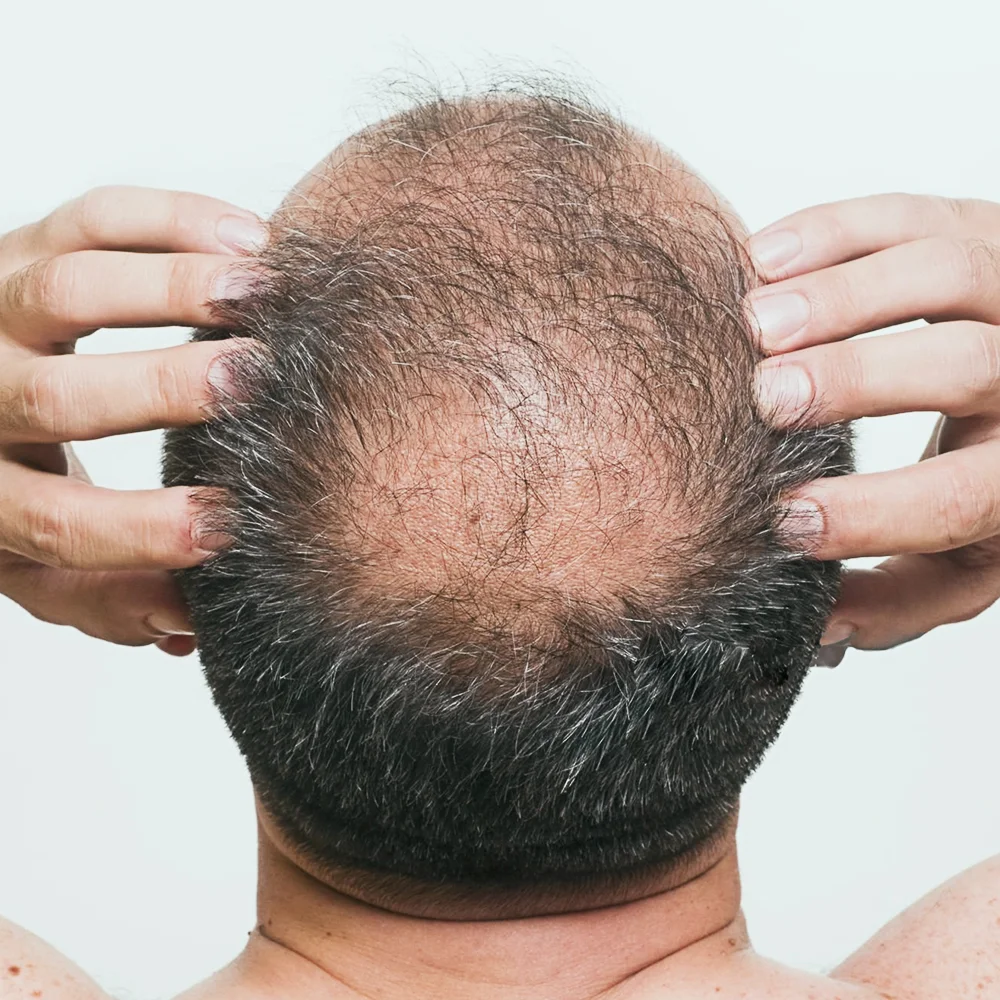
Also known as “male-pattern hair loss”, Androgenetic alopecia is the most common cause of hair loss in men. Genetic factors play a major role. Therefore, a person’s risk of developing Androgenetic alopecia is higher if this condition runs in the family.
In genetically-predisposed men, the male sex hormones (also called androgens) cause premature involution (shrinkage and reduced activity) of the hair follicles. Involution of the hair follicles occurs in a slow and progressive manner over many years, decades, leading to gradual thinning of the hairs, and eventually baldness in some individuals. The hair follicles on the vertex(the top of the head) are most susceptible to the effect of androgens. Consequently, hair thinning tends to be most pronounced on the vertex. While most men will start to experience thinning of their hairs around their 40s-50s, some men with a strong family history of Androgenetic alopecia will start to experience this at a younger age. Treatments are available to slow down the thinning process and to stimulate hair growth. Treatment is more effective if started early. Treatments that are evidence- based (backed by robust scientific evidence) include:
- Topical Minoxidil
- Oral Finasteride tablet (androgen blocker)
- Low level Laser Light therapy
If the above treatments do not provide satisfactory results, one can consider hair transplantation procedure.

Many women are afflicted with hair loss and hair thinning problems. There can be multiple causes. Genetic factors, stress, deficiency in certain key nutrients, dramatic weight loss and hormonal imbalance are common causes of hair loss in women. It is advisable to consult a medical professional early to determine the underlying cause of your hair loss problem. Female pattern hair loss is thought to be the female version of “androgenetic alopecia”. This is the most common cause of hair loss in women. It causes gradual thinning of hair on the vertex of the scalp, resulting in a widened parting line. Treatment for female pattern hair loss include:
- Topical Minoxidil
- Oral Spironolactone
- Low Level Laser Light Therapy
If results from the above treatments are unsatisfactory, one can consider hair transplantation procedure.
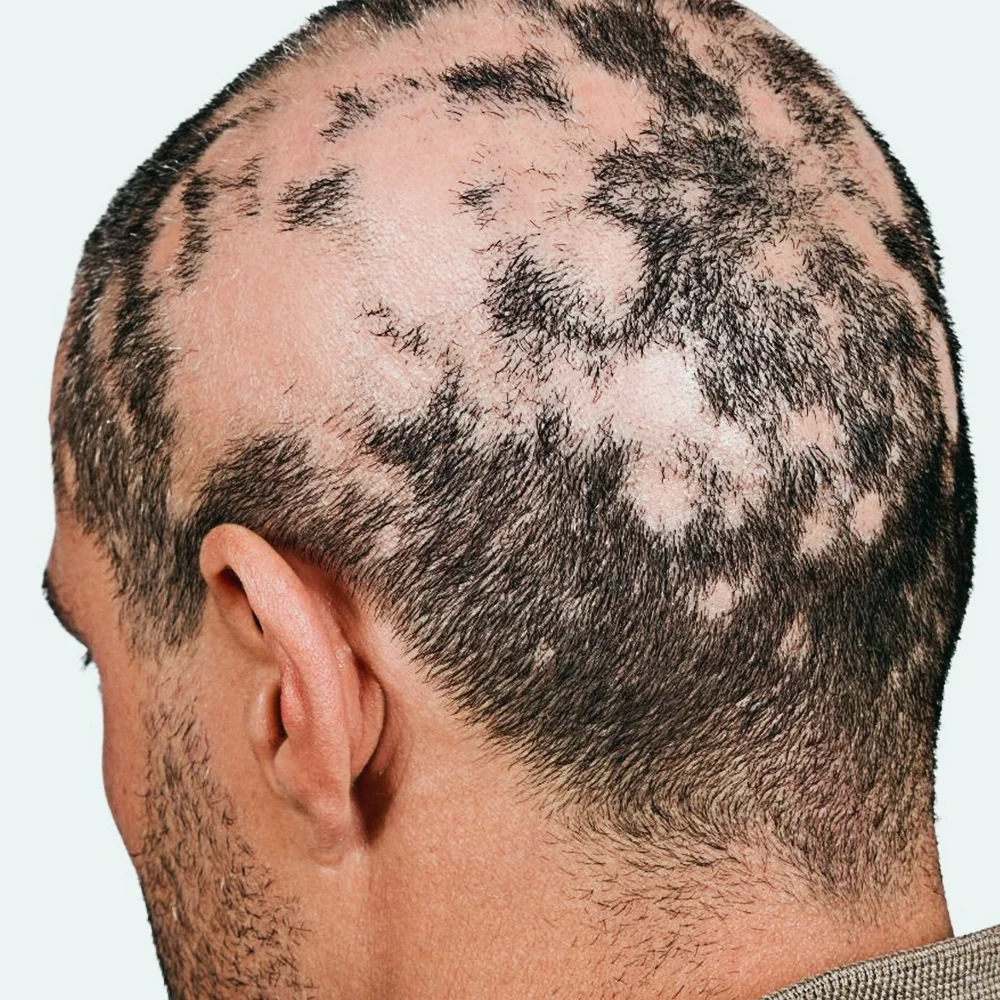
Alopecia areata is an auto-immune condition that can affect children and adults. It causes a discrete circular patch or multiple discrete patches of hair loss. Alopecia areata is caused by immune-mediated attack on the hair follicles.
Treatment for Alopecia areata include:
- Topical steroids
- Intralesional steroids (steroid injections)
- Topical minoxidil
- Immunotherapy
- Oral immunosuppressive therapy

Acute Telogen effluvium is a condition characterised by sudden increase hair fall / diffuse shedding of hairs. Our hair follows a growth cycle of 3 recognised phases:
Anagen- growth phase
Catagen- transitional phase
Telogen- Resting phase
The hair shedding is usually delayed- occurring around 4 weeks after the stressful event. Acute Telogen effluvium is a short-lived condition. Spontaneous complete recovery is expected after 6 -8 weeks.
Common Skin Infections
We discuss about common skin infections below.
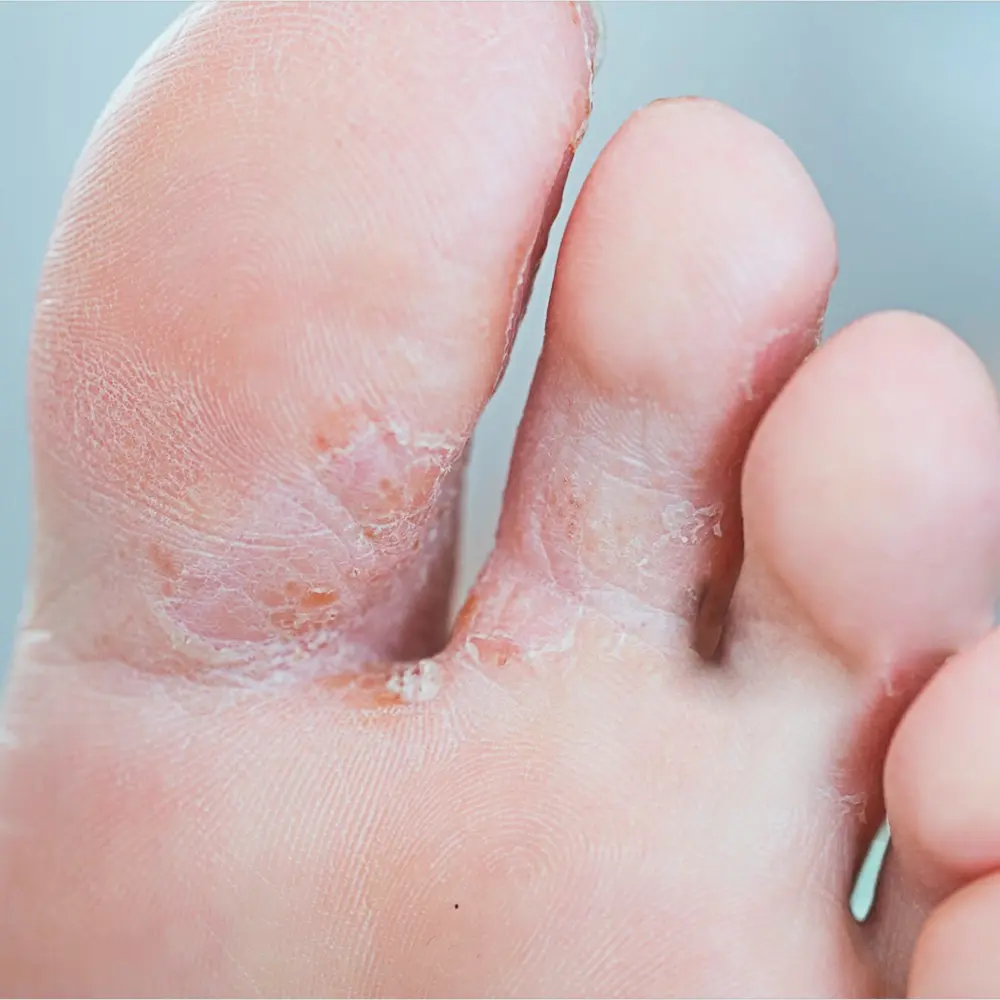
Also known as “ringworm”, Tinea is a common fungal skin infection. It tends to occur on the feet, groins and buttocks. The rash may appear “ring” like. Blisters may occur too. Tinea can be treated with topical and/or oral antifungal medications.
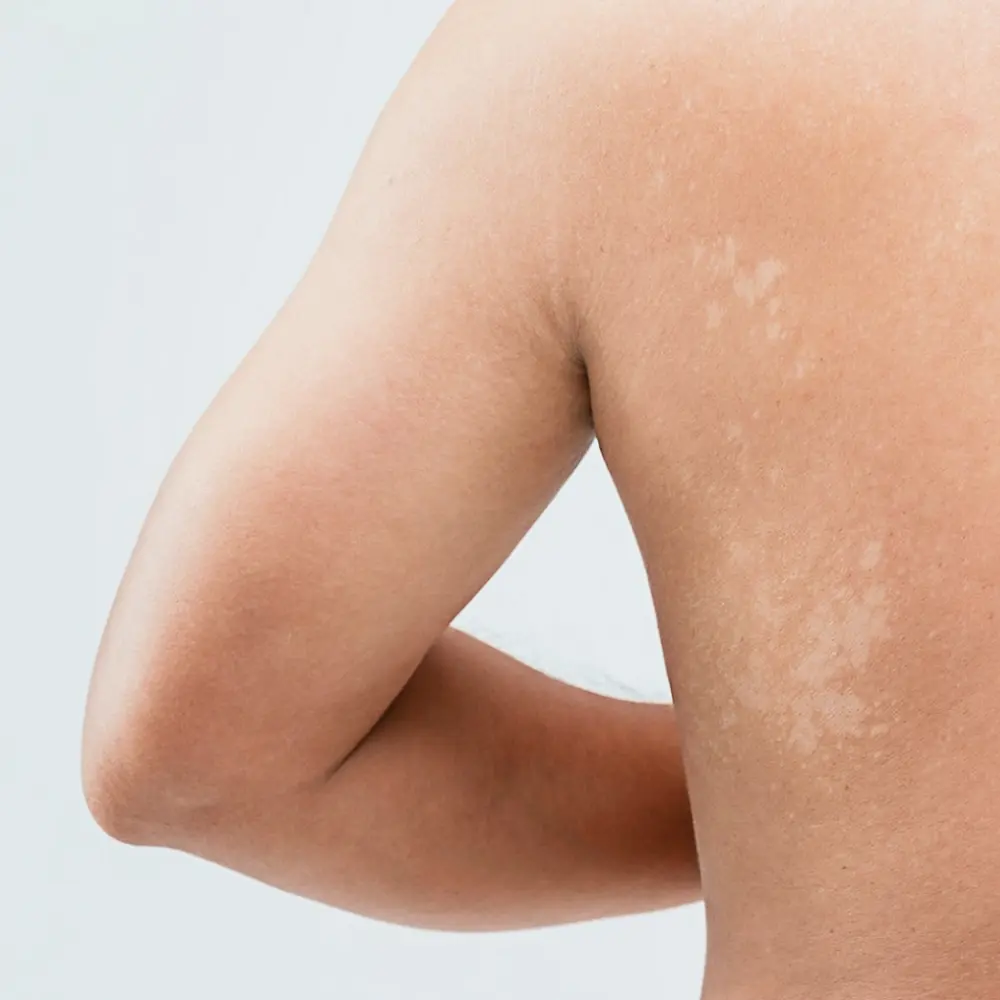
This is a skin infection caused by overgrowth of a yeast organism: Malassaezia Furfur. It is triggered by warm weather and sweat. It leaves brown and white spots on the body. Pityriasis versicolour is treatable with topical antifungal preparations. For severe cases, oral antifungal medications are sometimes required.
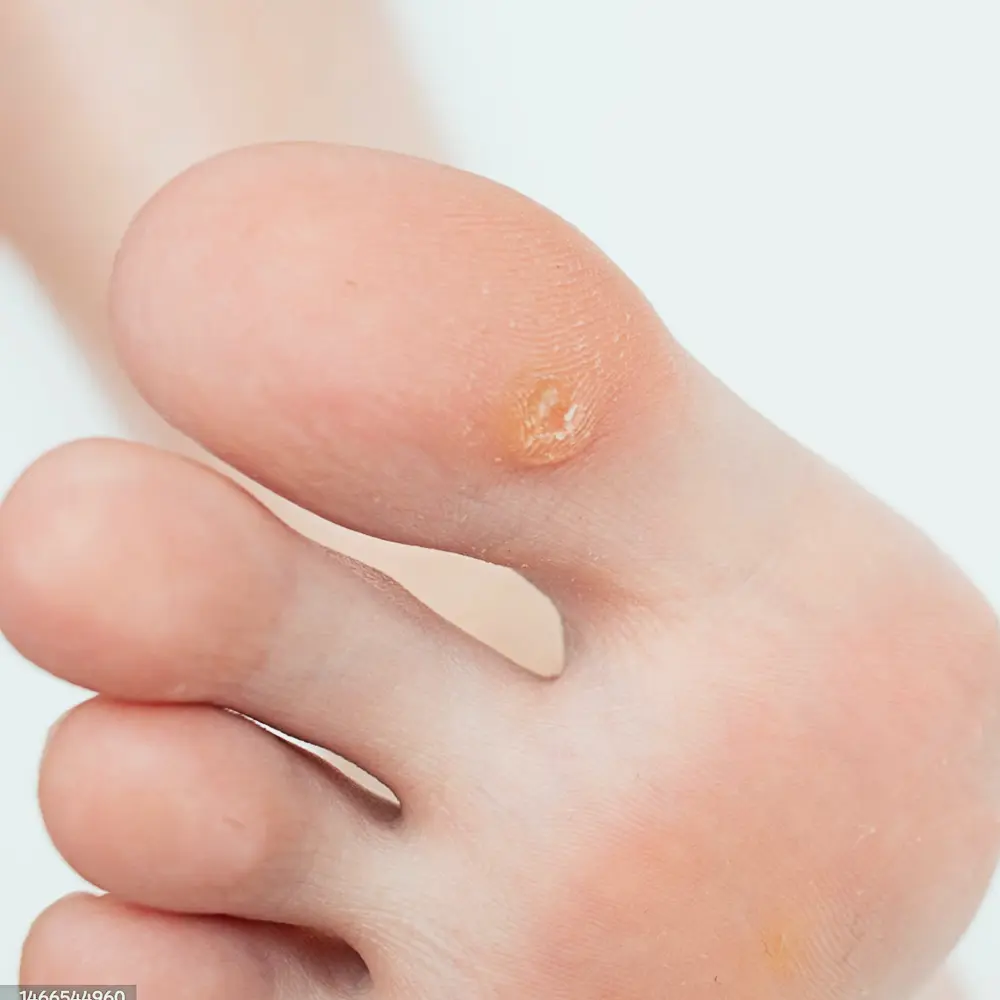
Viral warts are caused by the Human Papilloma Virus. It often causes bumps to develop on the hands or feet. If left untreated, they can spread. Viral warts can be treated with a variety of methods such as: topical medications, cryotherapy(liquid nitrogen), electrosurgery or lasers.
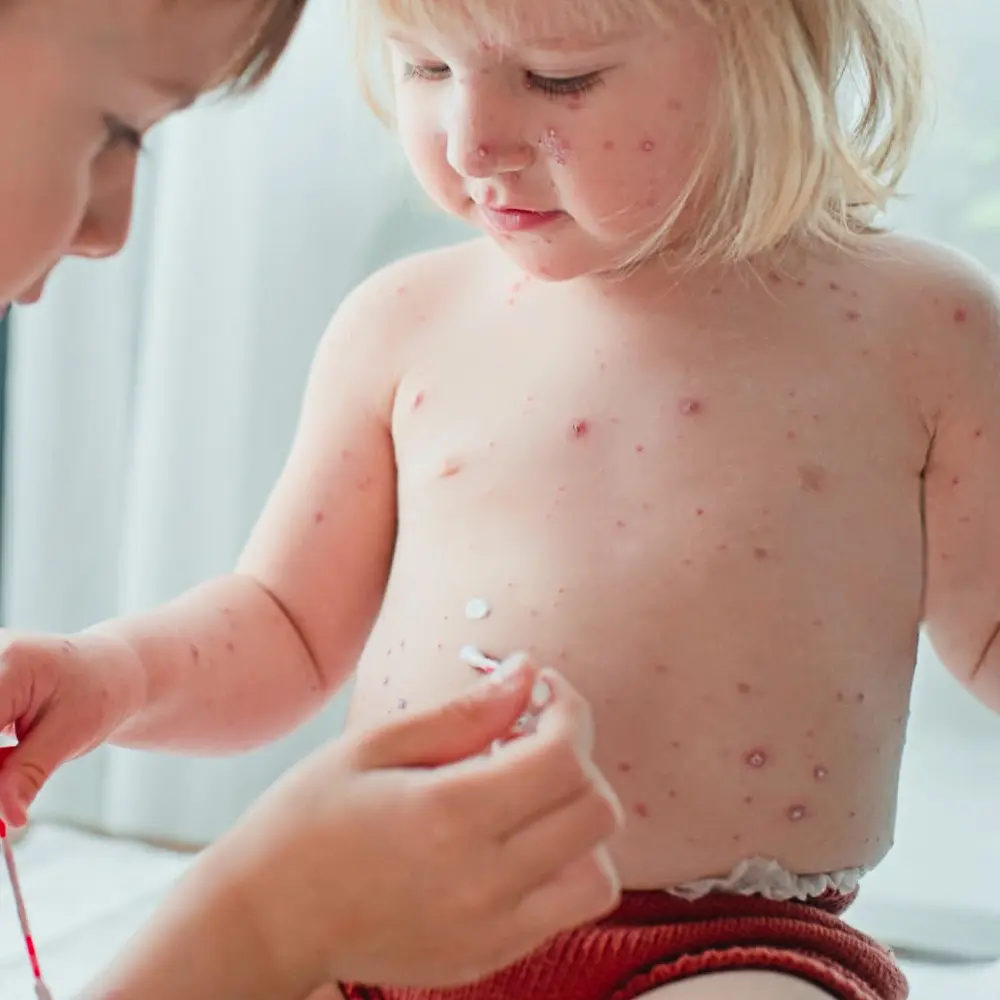
Molluscum is a common infection in children. It is caused by the Pox Virus. They appear as tiny, translucent bumps on the skin. It left untreated, molluscum can spread. It can be treated with a variety of methods such as: topical medications, cryotherapy(liquid nitrogen), or electrosurgery.

Herpes is caused by the Herpes Simplex Virus. This infection causes painful blisters and ulcers to develop on the skin. It commonly affects the lips and the private areas. Transmission of this infection is via skin contact. Once the infection is acquired, the body is unable to eradicate the virus and the virus can “reactivate” periodically, causing repeated episodes of blisters and ulcers. Antiviral medications are available for the treatment of Herpes.
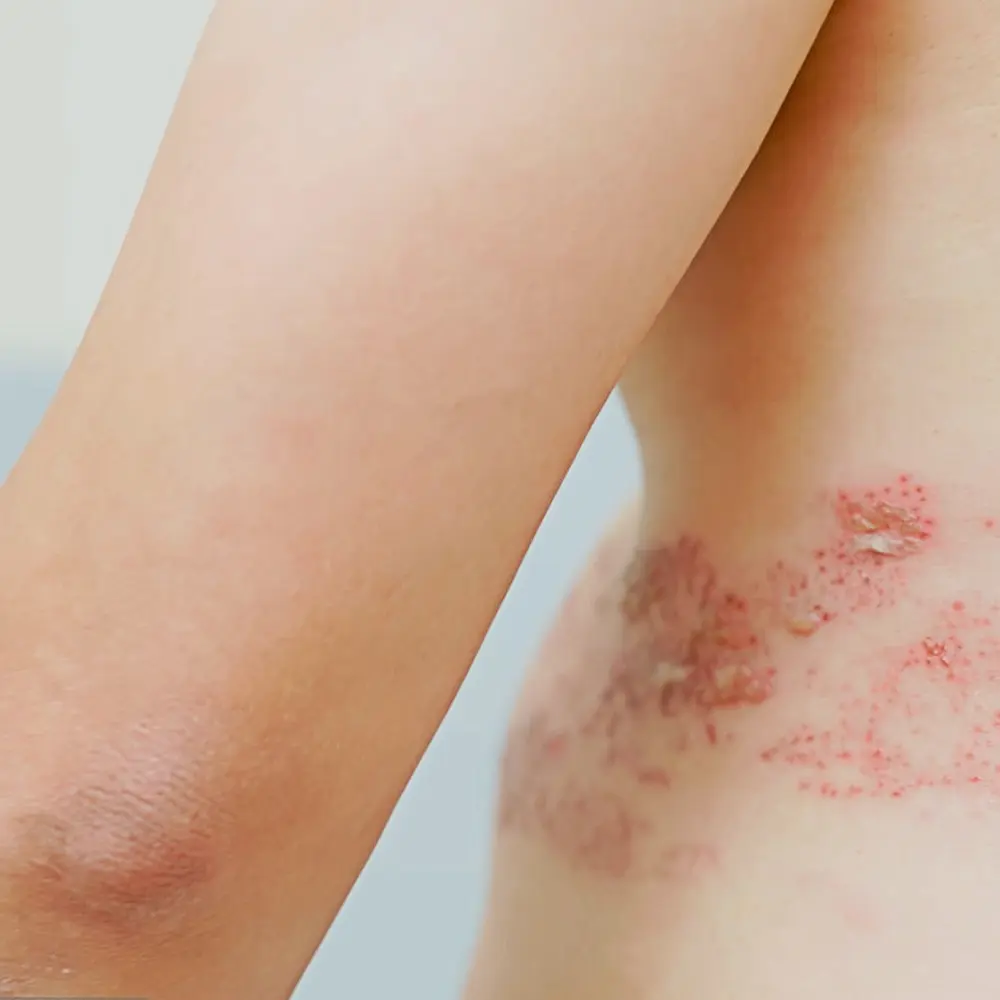
Shingles is caused by the reactivation of the Varicella Zoster Virus in the body. This virus is also the cause of Chicken Pox. Shingles causes painful blisters to form over a “band-like” distribution on the skin. Antiviral medications are effective in the treatment of Shingles. Seniors and individuals with low immunity are at risk of developing Shingles. Vaccines are available for the prevention of Shingles.
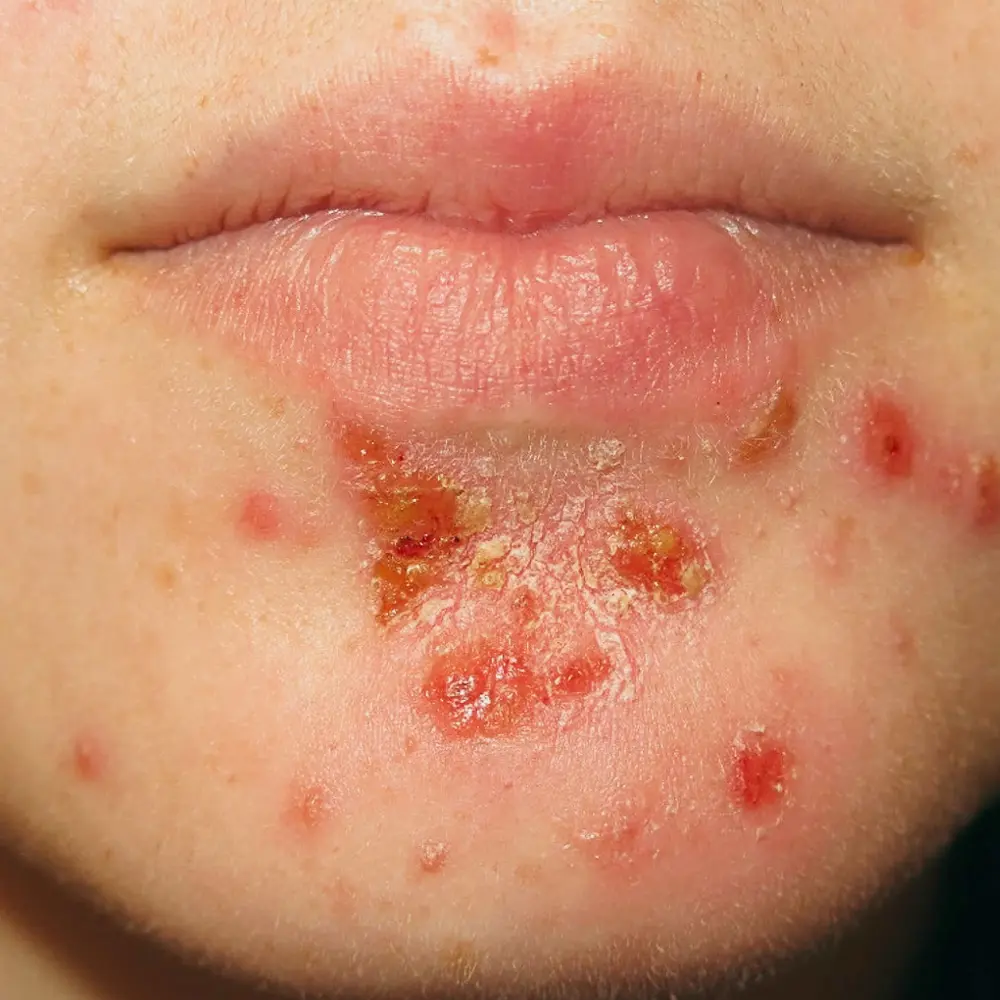
Impetigo is a common bacterial skin infection in children. It appears as weepy, crusted red plaques on the skin. It can be quite infectious and children in close contact can transmit the infection. Impetigo can be treated with oral and topical antibiotics.
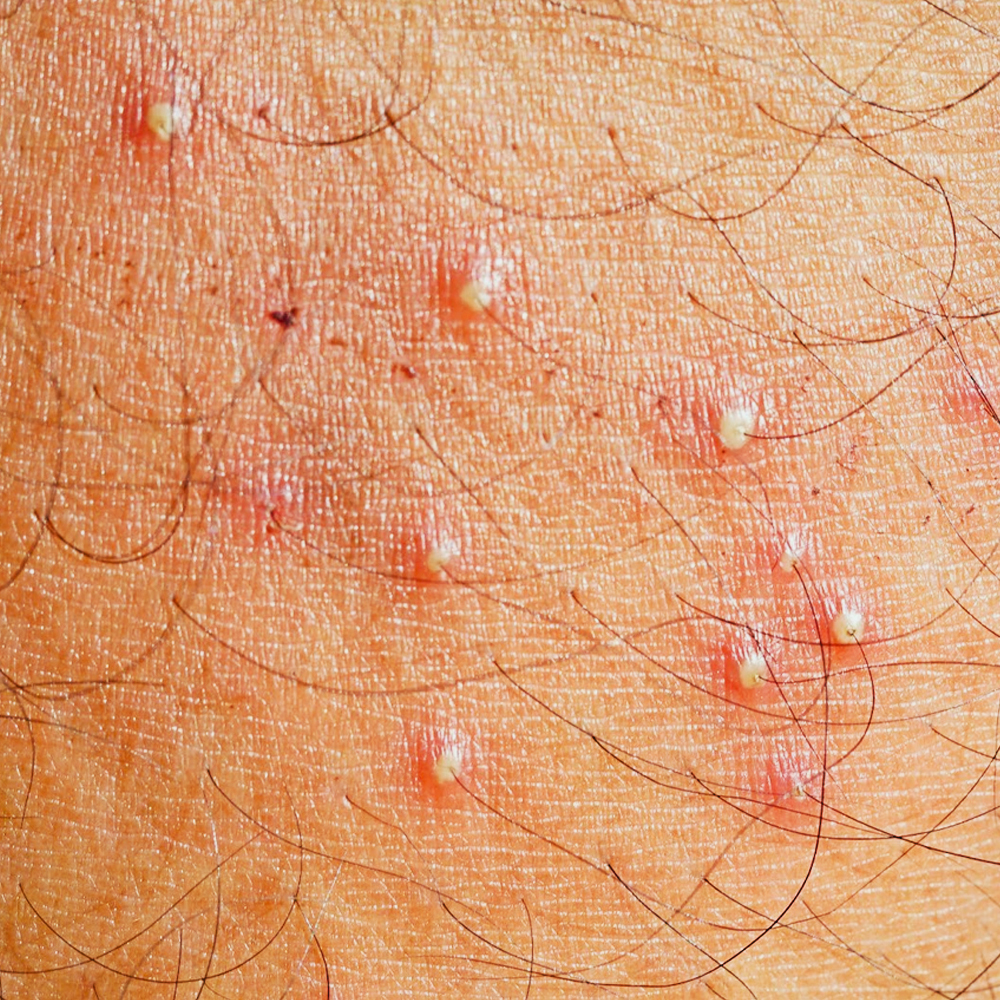
Folliculitis is an infection of the hair follicles. It causes small, pimple-like bumps on the skin. Hairy areas (eg the beard region, legs) as well as the upper back are more prone to developing Folliculitis.
Folliculitis can be treated with oral and topical antimicrobial agents.
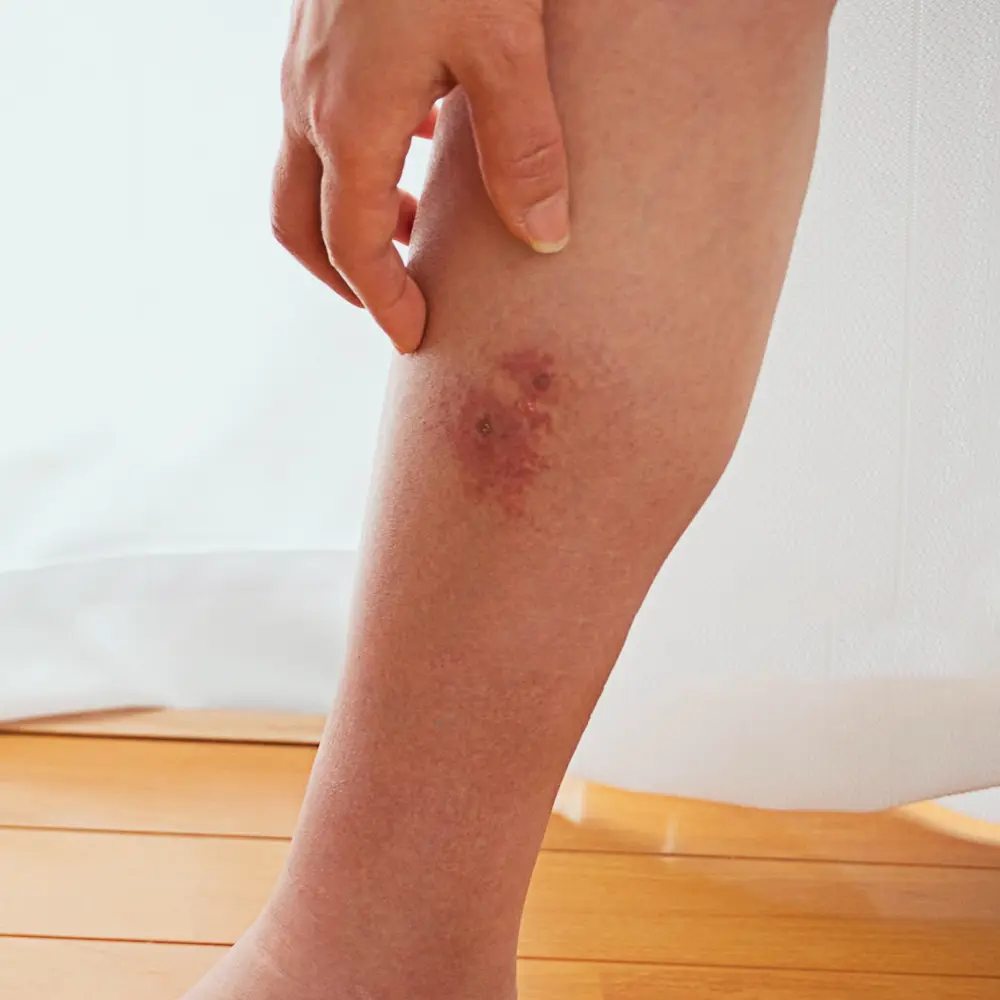
This is a common infection affecting the upper layers of the skin. It most commonly affects the legs. It causes painful, red patches, sometimes with watery discharge and blisters. Oral or intravenous antibiotics are required to treat this infection.
Psoriasis
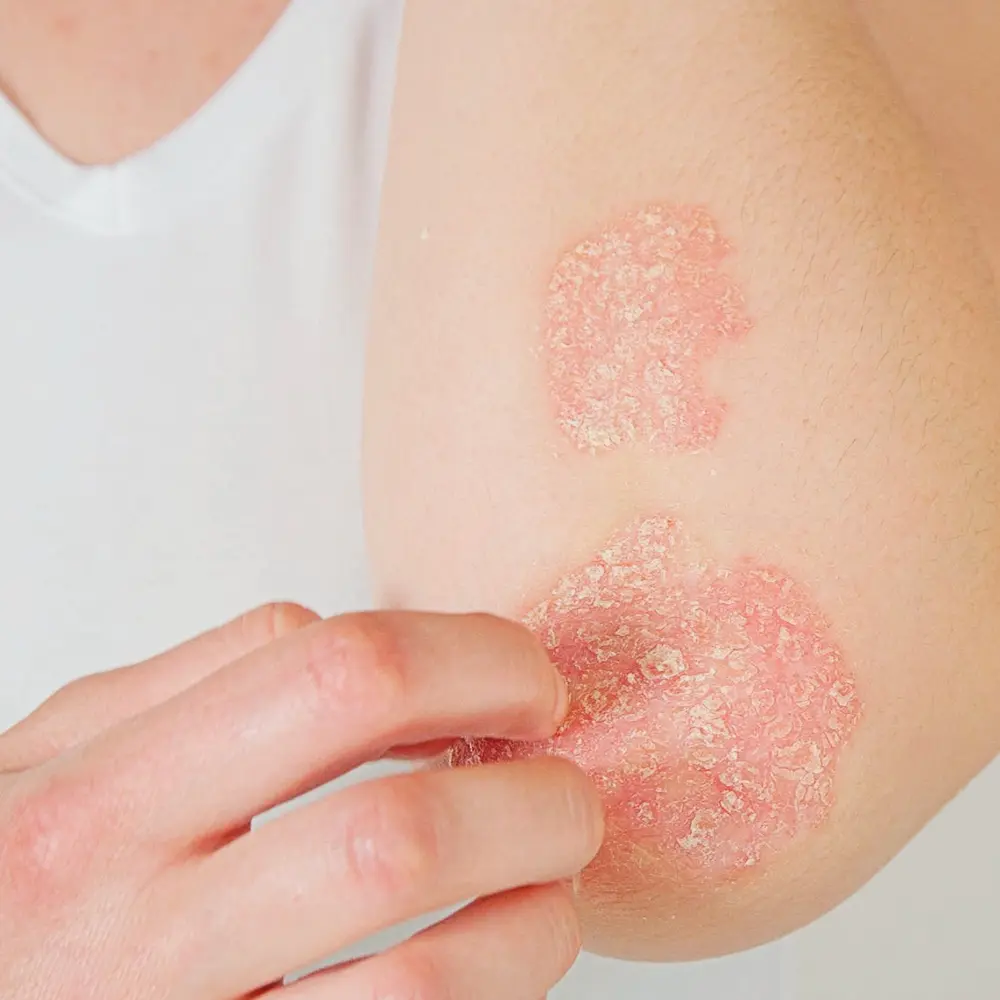
Psoriasis is a chronic, multi-system, immune- mediated inflammatory disease which frequently involves the skin, nails and joints. When psoriasis affects the skin, it causes pink scaly rashes which may or may not itch. Any part of the body can be affected but it tends to involve the scalp, face, elbows and knees. Psoriasis may be aggravated by factors such as: alcohol, infection( eg flu), stress, physical trauma to the skin ( eg rubbing/ scratching), and certain medications such as beta-blockers and ACE inihibitors. The disease may begin during childhood or early adulthood. Individuals with psoriasis have a higher risk of developing diabetes, heart disease, obesity and inflammatory bowel disease.
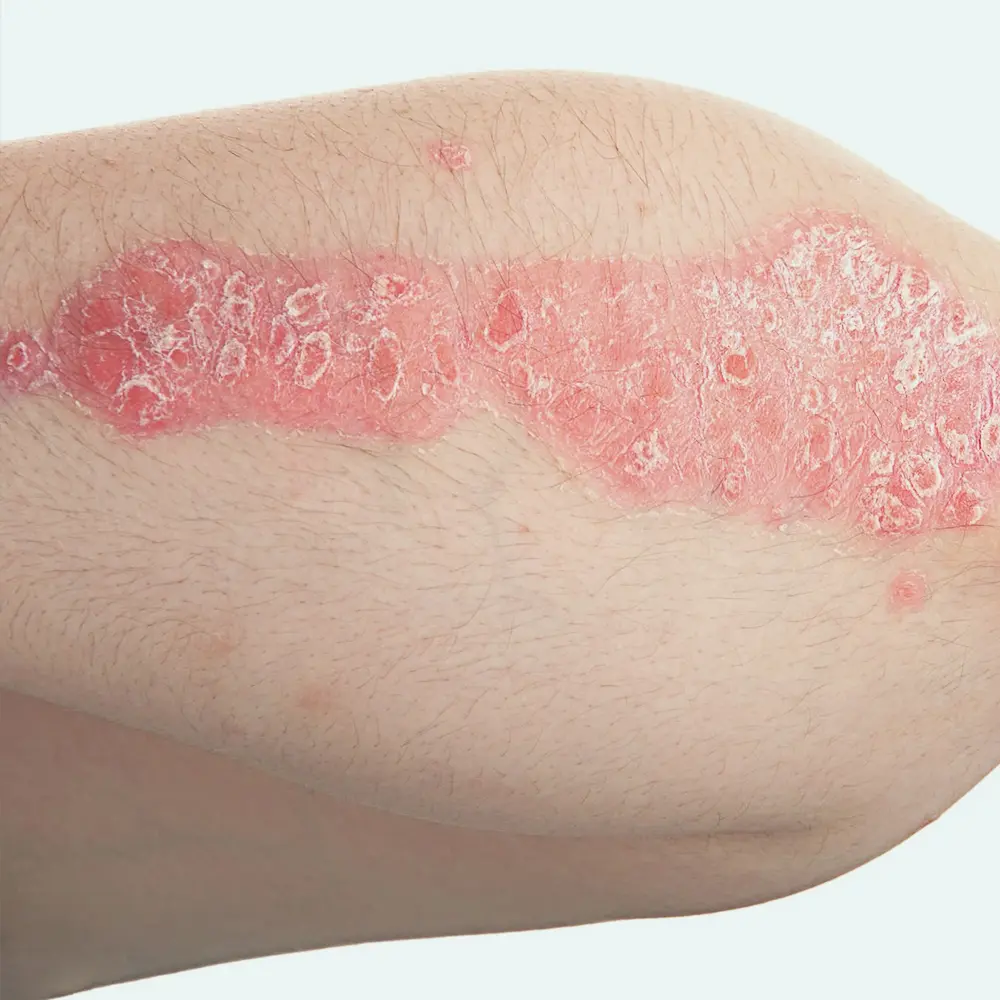
There has been a lot of research looking at the causes of this complex multisystem disease- current understanding suggests that Immune dysfunction and genetics are 2 major key drivers of psoriasis. Many different gene mutations have been implicated in the development of psoriasis.
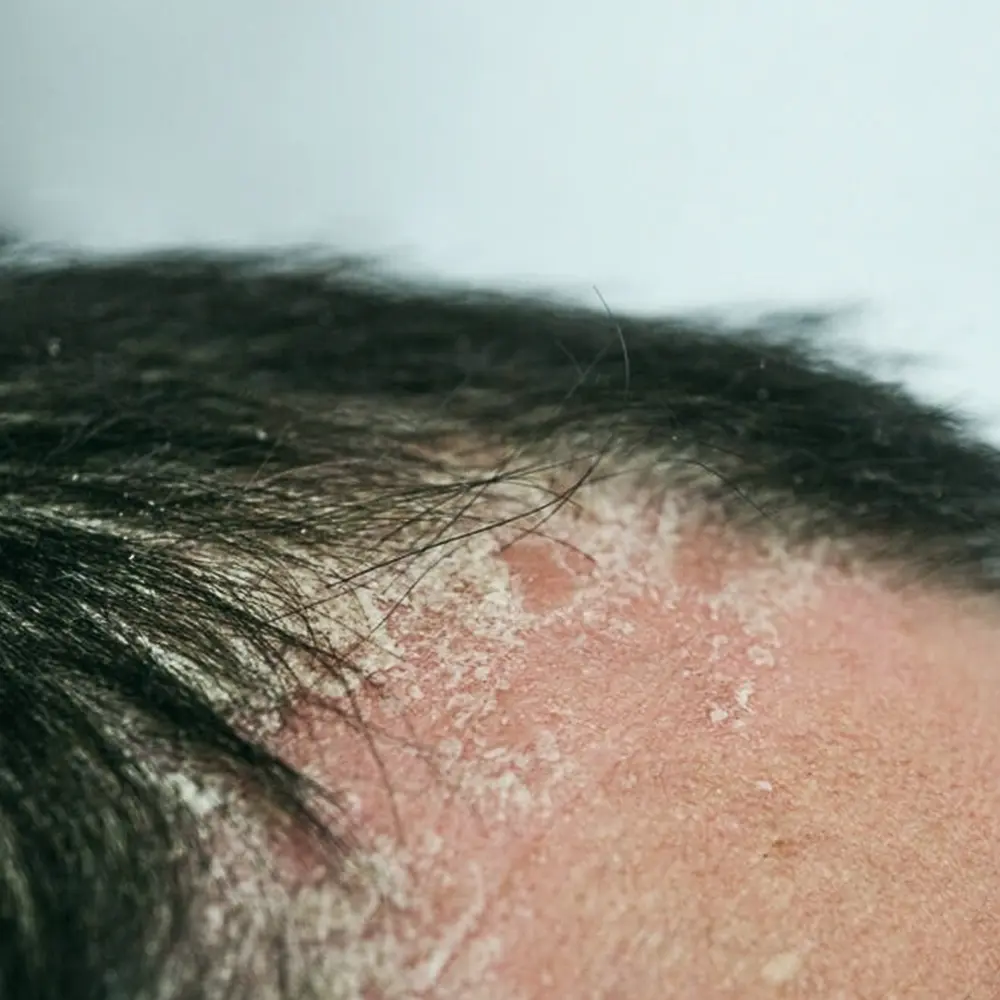
- Plaque Psoriasis (most common)
- Guttate Psoriasis
- Inverse Psoriasis
- Pustular Psoriasis
- Erythrodermic Psoriasis
- Palmoplantar Psoriasis
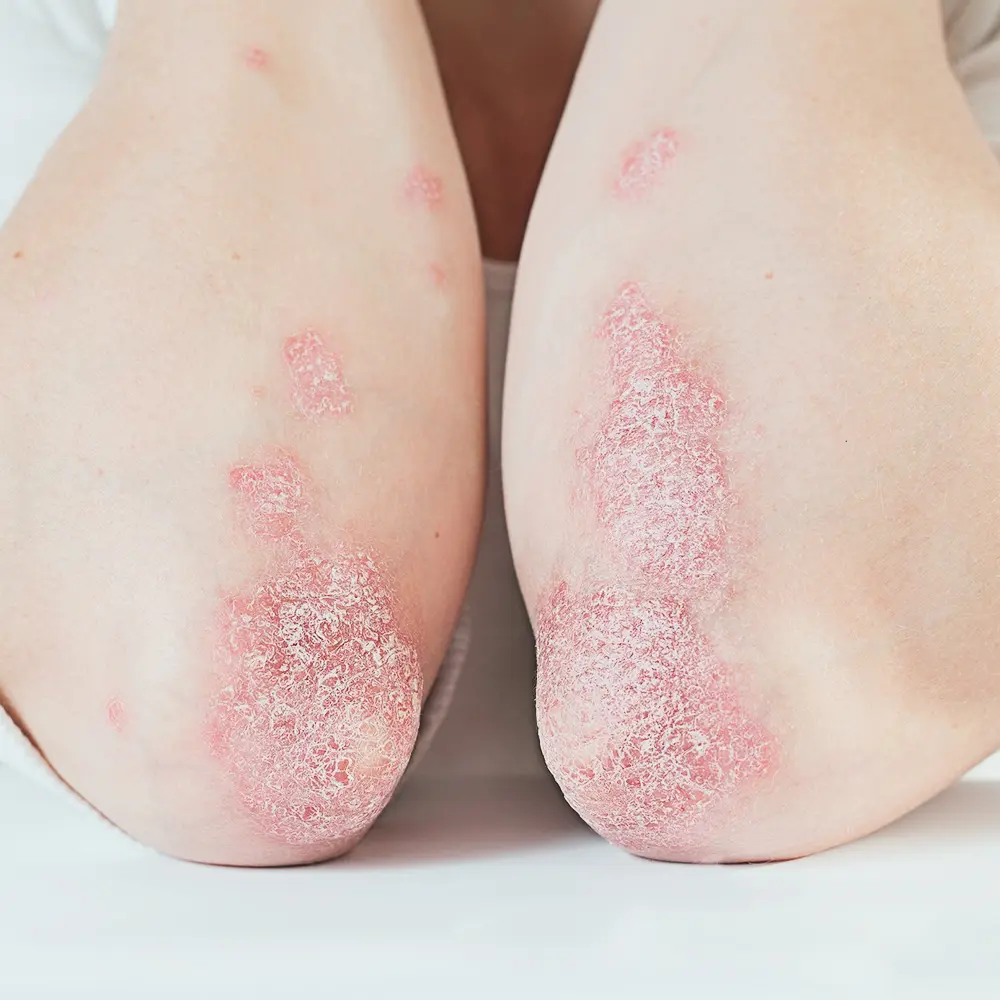
Psoriatic arthritis occurs in around 30% of patients with psoriasis. Some patients have psoriasis for many years before developing arthritis. Psoriatic arthritis can affect either the spine/shoulder/ hip joints , or the smaller joints of the arms and legs. Sometimes, the inflammation affects the ligaments/ tendons attached to the joints. Common symptoms of arthritis are: pain, swelling and stiffness.
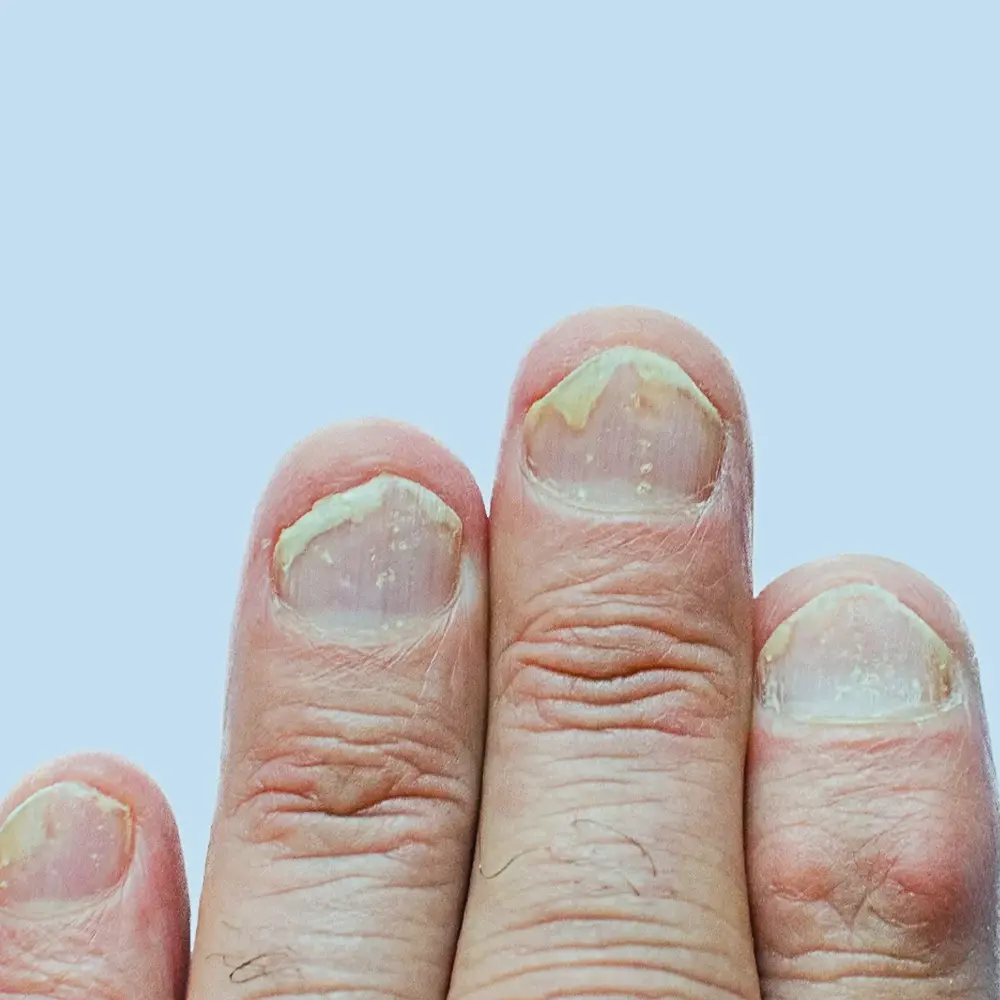
Psoriasis can make the nails look abnormal. Features of nail psoriasis:
- Thickening of the nail
- Pitting (like orange skin)
- Yellow-brown spots under the nail
- Onycholysis- separation of the nail from the skin beneath
There is a wide variety of treatments options for psoriasis, and treatment needs to be customized according to each patient’s profile and disease severity. The treatments can broadly be categorized into the following groups:
- Topical treatments ( eg coal tar, steroids, vitamin D3 analogues, calcineurin inhibitors
- Phototherapy
- Traditional Systemic treatments ( cyclosporine, methotrexate, acitretin etc)
- Biologic treatments
- Small molecules- eg JAK inhibitors
Eczema in Babies and Children
If you are a parent struggling to care for a child suffering from eczema, you are not alone. About 1 in 5 children in Singapore suffers from Eczema, which is also known as “ Atopic Dermatitis” .
Eczema is a chronic inflammatory skin disease which often starts during infancy or early childhood. Common triggers in children include: heat, sweat, infections ( eg coughs and colds) and vaccinations.

Common symptoms include:
- Itchy, scaly red patches
- Itchy red Bumps
- Dark and/or light coloured patches of skin- especially in Asians with darker skin tones
Common sites: In infants, eczema tends to affect the cheeks, elbows, ankle region and body. As the child becomes older, the eczema shifts to areas such as the skin folds eg neck, front of the elbows and back of the knees. Eczema commonly affects the eyelids too.

Eczema may be complicated by infection. Warning signs of an infection are: weeping/ yellow crusts/ blisters or pustules on the skin. It is important to seek medical attention promptly when a skin infection is suspected as oral medications and appropriate topical treatments should be promptly started.

The cause of eczema is complex and multifactorial. It is a chronic inflammatory skin disease where hereditary or genetic factors play a strong role, leading to an impaired skin barrier and immune dysfunction, causing dry, sensitive skin which is prone to recurrent inflammation and itch.

Although food allergy is more common in young children who suffer from severe eczema, it is not the main cause of eczema. Some signs of food allergy are: Aggravation of the skin symptoms soon after consuming the allergenic food/foods, and other symptoms such as hives, swelling of the lips/face, breathing difficulty, diarrhoea and vomiting after consuming the allergenic food/foods.

Acne
Acne is a common inflammatory condition of the oil glands which affects pre-teens, teenagers and young adults. It typically starts during puberty when the rise in sex hormones causes increase in oil gland activity. This leads to development of oily skin, clogged pores and pimples.
Female Adult Acne is another well recognized condition. Many females in their 20s, 30s and even 40s still struggle with acne. Female acne sufferers often experience cyclical outbreaks of acne which occurs around the time of their periods, reflecting the effect that female hormones exert on the oil glands.

The cause of acne is multifactorial. Genetic factors, hormones and bacteria are important factors. Normal healthy skin cells go through a self-renewal cycle around every 6 weeks: as new skin cells are formed, older skin cells mature, die and spontaneously shed off. However, in acne-prone skin, this skin renewal process is disordered. Dead skin cells tend to stick around and are unable to shed off, causing blockage of pores. The blocked pores then lead to build up of oil and overgrowth of bacteria, resulting in acne.

Mild acne can usually be treated with topical treatments that contain anti-bacterial or pore-unclogging ingredients such as salicylic acid, benzoyl peroxide, sulphur, niacinamide and resorcinol.
For moderate to severe acne, more potent prescriptive topical treatments may be needed. Oral medications can be very helpful too. They include: antibiotics, anti-androgens (suitable for females only), and oral isotretinoin. These medications need be used under medical supervision.
Apart from topical and oral medications, clinic-based procedures such as blue light therapy, deep cleansing facials, chemical peels and Intense Pulsed Light can also help to speed up clearance of acne and lighten acne scars.
Acne scarring can be prevented by early, effective treatment of acne. Therefore, it is highly recommended for acne sufferers to get treatment early. One should not wait to “out-grow” acne.

Pigmentation
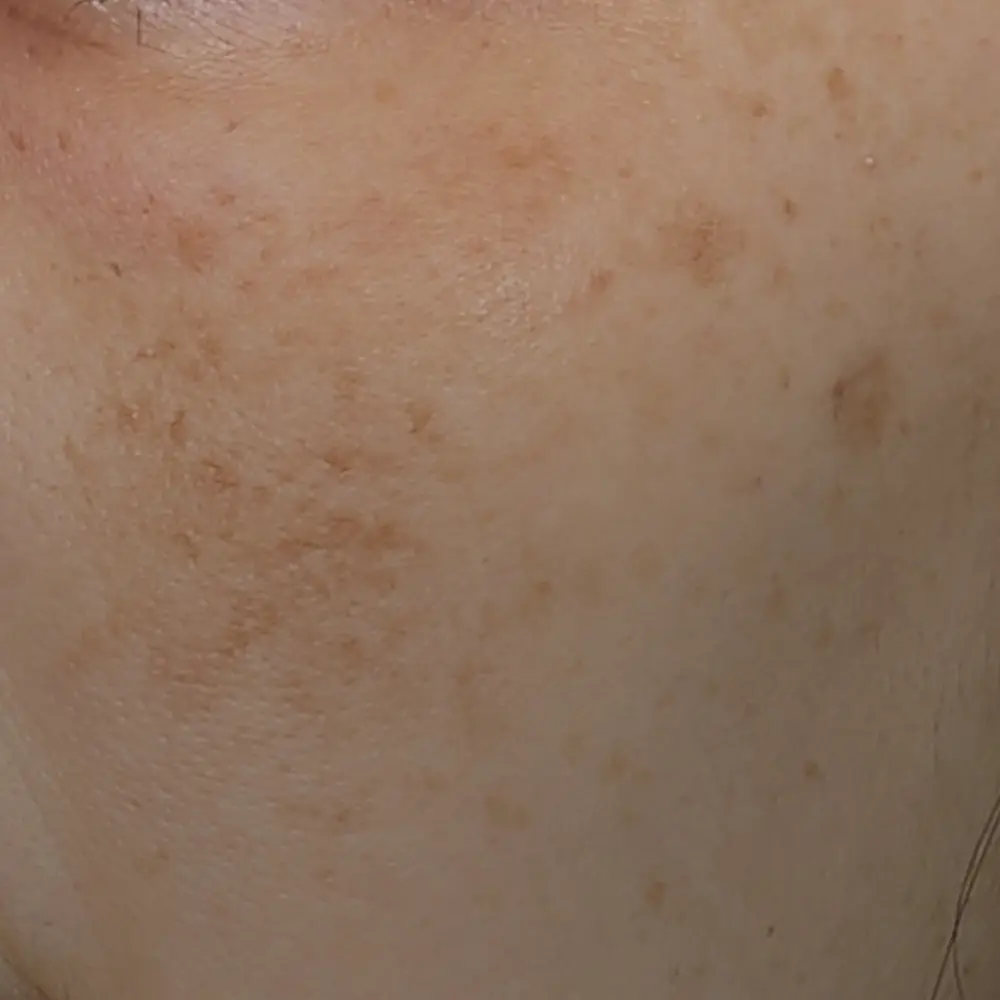
Pigmentation on the skin usually appears during middle age. Sun exposure plays a key role and in some individuals, hormonal and genetic factors also play a part.
There are different types of pigmentation issues, some of which require different solutions. There is no one-size- fit- all solution, and many over-the-counter skin whitening treatments have limited effectiveness. At W Skin and Laser Clinic, our dermatologist’s approach to dealing with pigmentation problems is first: to ascertain the correct diagnosis.
We discuss common pigmentation problems below.

Freckles are small light brown spots which are usually found on the cheeks of fair-skinned individuals. They can also occur on the rest of the face and body. They tend to appear at a young age and typically darken after sun exposure. Freckles can be effectively treated with sun-protection, topical whitening products, intense pulsed light or pigment lasers.

Lentigenes are small brown spots of variable sizes. They develop on the cheeks during middle age- around the 30s- 40s. They can be treated with sun-protection, topical whitening products, intense pulsed light or pigment lasers.

Melasma is a common pigmentation problem amongst Asian adults. They present as ill-defined brown patches or blue-grey patches on the cheeks and can also occur on other parts of the face eg forehead, nose, around the mouth. It sometimes develops in women during pregnancy or when a woman consumes oral contraceptive pills, due to the stimulation of melanocyte activity by female hormones. Unlike freckles and lentigenes, the response of melasma to laser treatments is variable and less predictable. Successful treatment of melasma often requires a combination approach of topical therapies, and sometimes oral medications and laser/ light based treatments. Strict sun avoidance and sun protection is very important.
Treatments that have shown favourable results for melasma include:
- Topical whitening treatments eg
- Hydroquinone / tretinoin containing preparations or “triple combination” preparations ( containing hydroquinone, tretinoin, steroid)
- Cysteamine
- Arbutin, Niacinamide, glycolic acids, Vitamin C
- Oral tranexamic acid
- Chemical peels
- Intense Pulsed Light and Lasers can be useful adjunctive treatments

Hori’s nevi is a pigmentation problem which is unique to people of Oriental descent. They appear as bluish-grey spots on the cheeks, usually during early adulthood. About 50% of cases affected have other family members having a similar problem. As the pigmentation in Hori’s nevi lie deep in the skin, topical whitening treatments, intense pulsed light and chemical peels are usually ineffective as these treatments can only reach the superficial skin layers.
Pigment lasers are highly effective in the treatment of Hori’s nevi as they are able to penetrate to the depth where the excessive pigments occur. Multiple sessions are usually required in order to achieve effective lightening/ clearance of Hori’s nevi.
Skin Care
At W clinic, we take pride in our range of skin pampering products that will cater to various skin care needs. W skin, our in-house medical-grade skin care range, is developed by our dermatologist based on the philosophy: CORRECT, PROTECT and REVITALIZE. Whether you are troubled by acne, pigmentation, or sensitive skin; or wish for a smoother and more radiant complexion, our products are formulated to help alleviate these problems and achieve healthy, great-looking skin.

This gentle wash cleanses skin perfectly in the gentlest possible way without drying and irritating. It dissolves keratin, purifies and keeps skin free of dirt and grime. It also helps to balance the biological equilibrium of skin’s functions, thus helping skin defend itself against external aggressions such as pollution. Day after day, skin appears more youthful and the complexion becomes fairer and more radiant.

This cleanser is the first step to healthy skin. It gently creates a clean and healthy environment free of surface impurities. Perfect for normal, oily and blemish-prone skin, the wash contains salicylic acid to unclog pores while organic Edelweiss extract botanicals condition, soothe and nourish the skin. It also helps to lighten the appearance of blemish-related pigmentation for a more even complexion.

Comfort irritated skin and perk up a fatigued-looking complexion with this light textured lotion which gently moisturizes as it reveals a brighter-looking skin tone. Featuring the skin-soothing complex – Allantoin, Butcher’s Broom, Centella Asiatica, Calendula and Horse Chestnut – it brings comfort to irritated skin and boosts the skin’s natural hydration levels over an extended period of time. Skin is refreshed, purified, quenched and soothed throughout the day.

This high-performing brightening treatment targets dark spots, freckles, and dullness to restore your skin’s luminosity. It lightens your overall complexion and enhances clarity plus glow. The remarkable formula works within skin and the combination of potent actives including niacinamide and alpha-arbutin provides an all-rounded solution to pigmentation. Skin is fortified and protected to restore glow from a dull, tired complexion.

This exclusive, super silky and non-greasy serum is powered by pure, potent actives designed to regain skin’s lightness and youthfulness. It helps to guard your skin against premature aging, discoloration and the cumulative damage induced by damaging free radicals and environmental aggressors. It may also help to promote essential collagen synthesis, leaving skin dewy, firm and more radiant, with better tone and texture.

One of our all time best-sellers, this light, quick absorbing serum contains encapsulated Retinol which is a time-tested anti-ageing ingredient, helping to stimulate skin cell renewal, minimizing fine lines and wrinkles, revealing a radiant, clear skin tone.

This non-greasy, ultra-light emulsion is the answer to complete protection from the sun’s noxious UV rays and other environmental pollutants. The spectacular blend of ingredients ensures tanning is effectively avoided, while providing full-spectrum shielding. Strengthened with vitamins C and E, skin enjoys an unsurpassed level of moisture and nourishment that helps keep it healthy. Skin feels velvety, smooth and light throughout the day!
SCAR TREATMENT
Scars occur as a result of skin injury. “Injury” to the skin can result from: traumatic injury, surgery, burns, or inflammation of the skin (eg acne).
Some scars may be aesthetically displeasing. Some scars may be itchy and painful.
There are a variety of treatments that can improve the appearance of scars, as well as reduce the itchy and painful symptoms of scars.
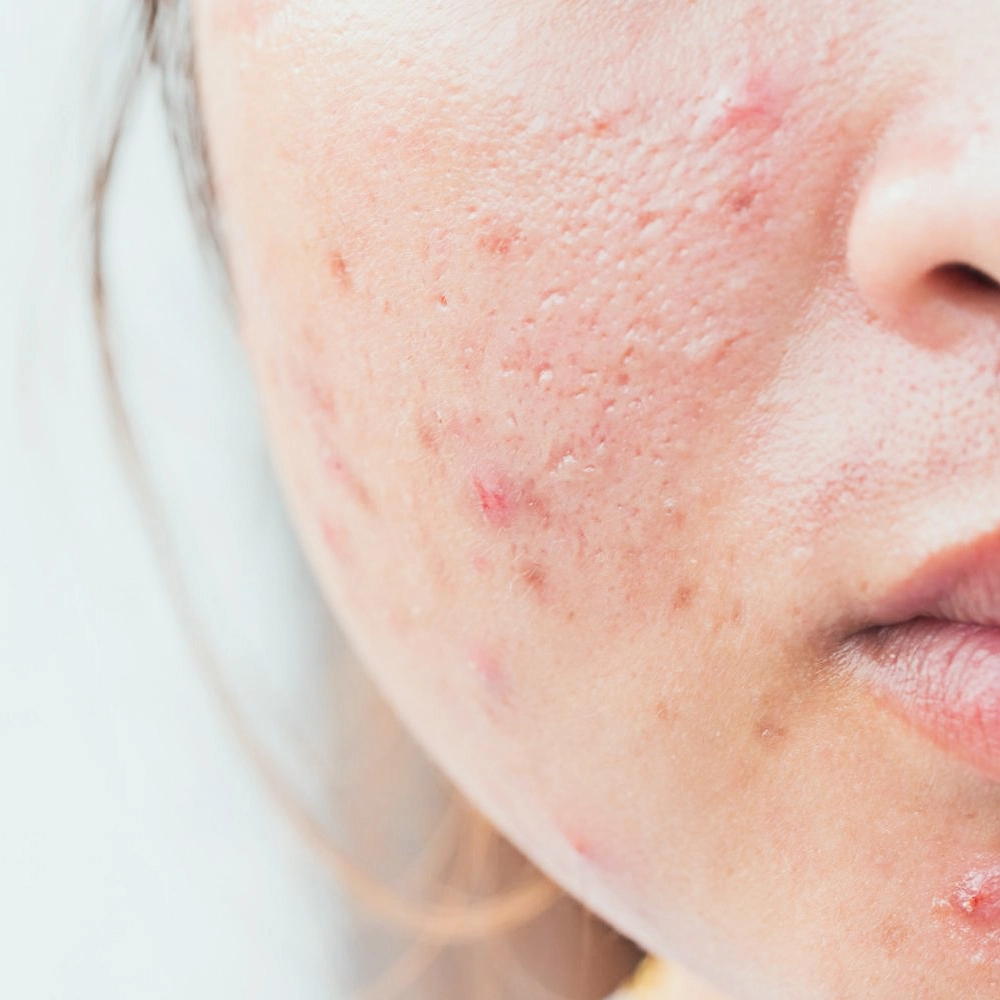
There are different types of acne scars. They can be divided into:
- Post inflammatory hyperpigmentation
- Atrophic scars
- Hypertrophic scars

Acne often leaves behind brown discoloration. This problem is common in individuals with darker skin tones and in people who repeatedly squeeze their pimples and manipulate their skin. Post inflammatory hyperpigmentation usually improves spontaneously over time but this may take many months or even years. It is important to avoid excessive sun exposure as this can aggravate the brown discoloration. Skin lightening creams and chemical peels can help to speed up the lightening of these scars.

Atrophic acne scars refer to depressed or “sunken” scars that occur post acne. These occur as a result of collagen damage caused by severe, prolonged, inflammatory or cystic acne.
To avoid development of atrophic scars, acne should be treated early.
Atrophic acne scarring can be improved with procedural treatments such as resurfacing lasers, subcision, filler injection, and scar revision surgery. Sometimes, a combination of the aforementioned treatments is required.

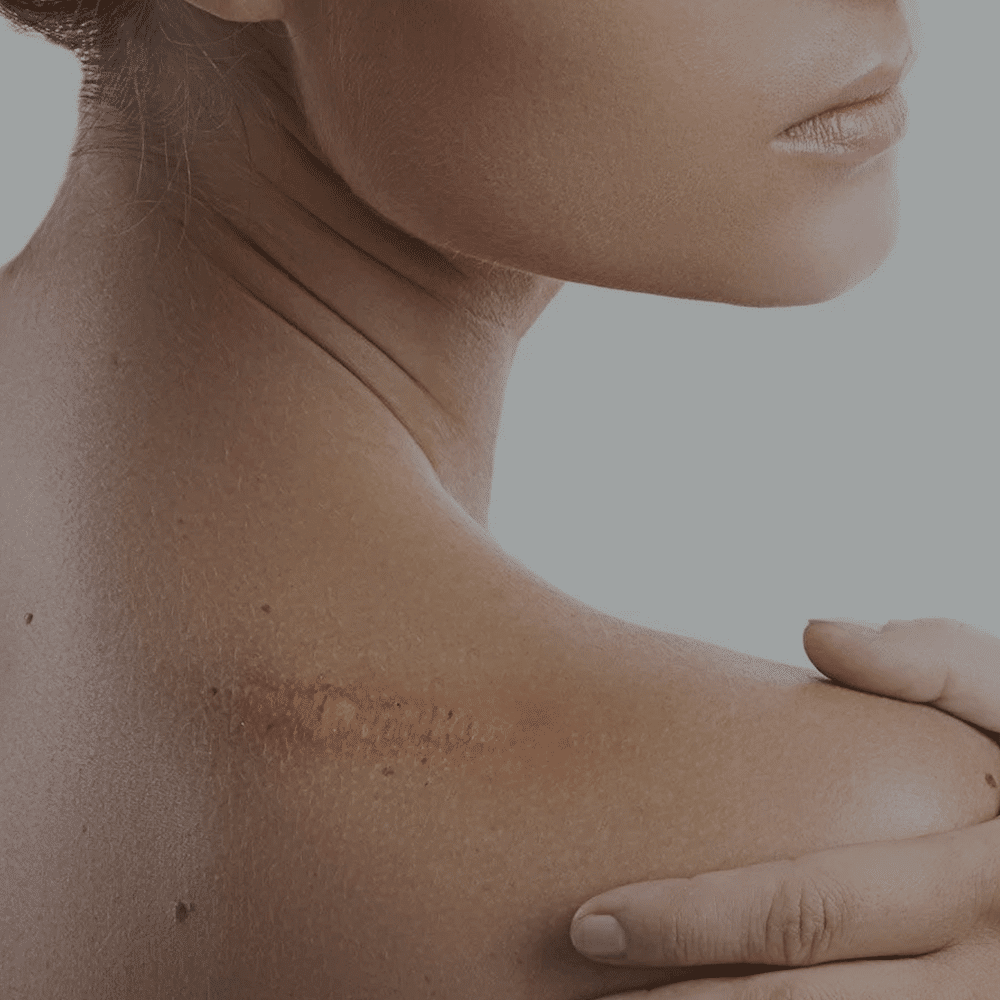
Hypertrophic scars and keloids are thick, bumpy scars. They can develop after surgery ( eg Caesarean- section), vaccinations, burn injury, acne, skin piercings or tattoos. The upper arms, upper back, chest and jawline are especially prone to hypertrophic scars and keloids. They can be red, itchy, painful or hypersensitive.
These scars can be treated with intralesional injections, lasers, medicated gels and silicon plasters. Selected patients will also benefit from scar revision surgery.
Skin Cancers
Skin cancers are one of the commoner cancers. Risk factors for developing skin cancers include:
- Fair skin- individuals with lighter skin tones are at higher risk than darker skin tones
- Skin that burns easily under the sun
- Excessive ultraviolet light exposure
- Taking of Immunosuppressive medications over a long period of time
- Old age
- A family history of skin cancer, or a personal history of skin cancer

- Changing skin growth
- Asymmetry in size, shape, colour
- Ulceration/ spontaneous bleeding
- Irregular border

1. Basal cell carcinoma
This is the most common but least aggressive type of skin cancer. It tends to occur on the face, and usually appears as a smooth, pearly bump with fine blood vessels on top. It may sometimes ulcerate.
2. Squamous cell carcinoma
This is less common but more aggressive than basal cell carcinoma. It usually appears on the face, arms and ears, as a reddish patch or a red lump with crust on top. It can sometimes be mistaken for psoriasis or eczema.
3. Melanoma
Melanoma is the most aggressive type of skin cancer. It carries a high risk of spreading beyond the skin if it is not diagnosed and treated early. It tends to appear as a mole, brown spot, black spot or freckle which changes in colour, size and shape over time. Melanoma can develop under the nails too, and will present as a black/brown blotch or band under the nail.

Consult a dermatologist for a skin check if you are worried about a skin lesion. After a thorough skin examination, your dermatologist may advise doing a skin biopsy if any suspicious looking skin lesion is detected.
For fair skinned individuals, or individuals with a history of skin cancer, it is advisable to undergo regular skin checks by a dermatologist.
Making an early diagnosis is beneficial as most skin cancers can be treated and cured if they are picked up early.

Skin cancers are usually treated by surgical removal. For some very early skin cancers, or precancerous skin growths, non-surgical treatments can be effective too. Non-surgical methods include: cryotherapy( liquid nitrogen), Imiquimod cream, and photodynamic therapy.

As ultraviolet radiation is the most significant cause of skin cancer, sun avoidance and sun protection are key to skin cancer prevention.
- Avoid engaging in outdoor activities when it is very sunny
- Practise good sun protection
- Cover up – hats/umbrella/ clothing
- Use a broad spectrum sunscreen of at least SPF 30.
- When engaging in outdoor sports, use a water and sweat resistant sunscreen
- Reapply your sunscreen after 3-4 hours to maintain its protection